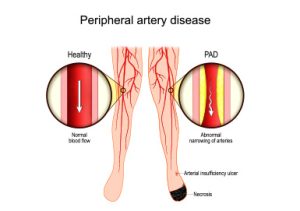
Peripheral artery disease (PAD) are a group of disorders characterized by narrowing of, or obstruction in, the arteries supplying to the hands and the legs. Atherosclerosis, the narrowing of arteries due to the deposition of fats in the wall, is the leading cause of PAD in individuals above the age of 40. Other causes of PAD are thrombosis, embolism, vasculitis, fibromuscular dysplasia, and trauma. PAD may also be an early warning of the deposition of fat occurring in the arteries supplying to other organs like the heart or the brain.
 Symptoms of peripheral artery disease
Symptoms of peripheral artery disease
Symptoms of peripheral artery disease (PAD) often include leg pain or cramping during walking, which improves with rest. Individuals may also experience numbness, weakness, or a cold sensation in the lower legs or feet. In severe cases, wounds on the feet or toes may heal slowly or not at all. PAD can also cause shiny skin, hair loss on legs, or weak pulses in the limbs.
- Pain, aching, and a sense of fatigue in your limb while exercising which gets relieved on resting (claudication)
- Aching and pain in your leg during sleep(when kept in a horizontal position), and relief when kept in a vertically downward position
- A feeling of numbness or cold in your foot or toes compared to the other leg
- Ulcers in your leg that won’t heal
- Reduce growth of hair in the affected limb compared to the other limb
- The slow growth of toenails in the affected limb
- Shiny skin on your affected leg
- Change in color of your leg
 Causes of peripheral artery disease
Causes of peripheral artery disease
- Atherosclerosis (deposition of fats and cholesterol into the wall of your arteries leading to a narrowing of its lumen, which in turn reduces the blood flow)
- Smoking
- Diabetes
- Hypertension
- High blood cholesterol levels
- Renal insufficiency
- Family history of stroke or heart disease or PAD
- Age over 50
How peripheral artery disease is diagnosed?
To diagnose PAD your doctor will first like to do a thorough physical examination in which might include looking for pulses in different parts of your limb, listening to the pulse with a stethoscope, and looking for signs of reduced blood supply, like change in color of your leg or ulcers which aren’t showing signs of healing. Other tests that your doctor may order are:
- Ankle: Brachial Index (ABI)
- Treadmill test
- Ultrasound
- CTA
- Angiography
Peripheral artery disease treatments
Your treatment will depend upon the severity of your symptoms. The treatment aims to prevent cardiovascular events, improve limb symptoms, and reduce the risk of developing critical limb ischemia.
- Discontinuing cigarette smoking
- Supervised exercise training for 30-40 minutes, 3-5 times a week for at least 12 weeks, for patients with claudication, led to an improvement in symptoms
- Control of blood pressure by taking antihypertensive medications like ACE inhibitors.
- Statins: for maintaining a normal lipid profile. (an abnormal lipid profile leads to increased risk for the development of PAD)
- Anti-coagulant therapy: aspirin or clopidogrel are prescribed to reduce the chances of lot formation which may narrow the artery
Cilostazol: increases the blood supply to the limb by dilating the artery
Pentoxifylline: increases the amount of oxygen that the tissue receives, hence partially compensating for the narrowing of the artery
- Percutaneous Transluminal Angiography (PTA): a small tube(catheter) with a balloon is inserted into the narrowed artery, the balloon is then inflated to flatten the fat deposit narrowing the artery. In some cases, your doctor might also put a stent in the artery to ensure that it remains open.
- Bypass surgery: your doctor might choose to create a new path for the blood to flow around the affected area with the help of a graft. The graft can be a vessel from your body or it could be made from a synthetic material.