Summary – When it comes to choosing a treatment for varicose veins, the decision between Radiofrequency Ablation (RFA) and VenaSeal can be difficult. RFA involves using heat to close off the vein, while VenaSeal uses a medical adhesive to seal it shut. While both treatments are effective, there are some differences to consider. Read this article to know the key differences. Ultimately, the choice between RFA and VenaSeal will depend on individual preferences and the specific needs of the patient.
Varicose veins don’t just look unpleasant. For many people, they cause real discomfort including leg heaviness, dull aching, swelling that builds up through the day. At some point, compression stockings stop being enough, and treatment becomes the logical next step.
Two options come up most often: radiofrequency ablation (RFA) treatment and VenaSeal treatment for varicose veins. Both treatments close off the damaged vein. Neither requires a hospital stay. But they work differently, and that gap matters more than most people realize when they’re sitting in a consultation room trying to decide.
What Actually Happens During Each Procedure
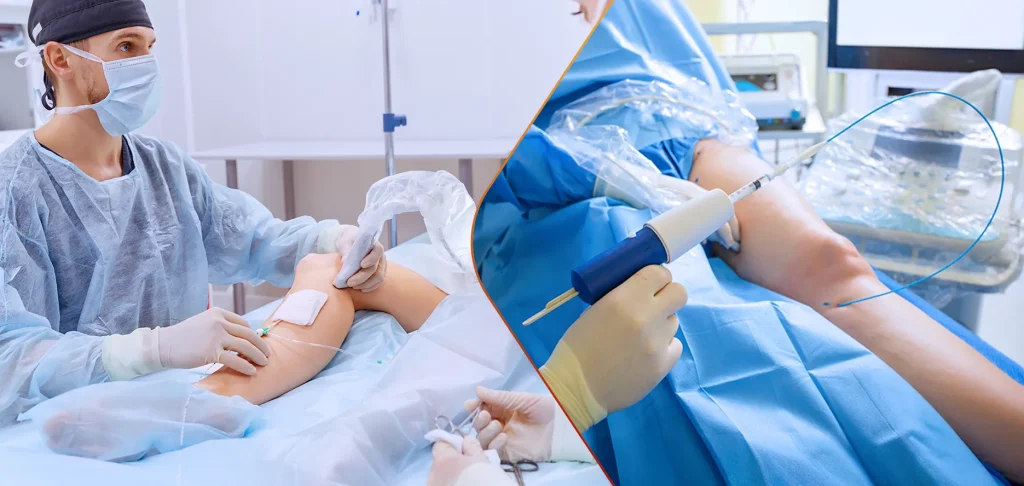
RFA treatment for varicose veins uses heat. A thin catheter goes into the vein, radiofrequency energy travels through it, and the vein wall collapses and seals shut. The body absorbs it gradually. Blood finds a better route.
It’s been done this way for over 20 years. That longevity isn’t just a selling point – it means there is a real outcome data to look at. Five-year success rates range from 90% to 98%. For a minimally invasive procedure, that’s a strong record.
VenaSeal skips the heat entirely. It uses a medical-grade cyanoacrylate adhesive, essentially a safe, surgical glue, to seal the vein from the inside. No thermal energy, no heat-related discomfort during recovery.
VenaSeal treatment for varicose veins has about a decade of clinical data behind it. Five-year success rates come in around 94% to 95%, which is comparable to radiofrequency ablation (RFA). The long-term picture beyond ten years is still being studied, and that’s worth knowing upfront.
Where the Two Treatments Actually Differ

Both procedures are done under local anesthesia on an outpatient basis. Most people return to normal activity within 24 to 48 hours. On the surface, they sound nearly identical.
The differences show up in recovery.
After radiofrequency ablation, compression stockings are standard – usually worn for one to two weeks. Some bruising or tenderness along the treated vein is common. It fades, but it’s there. For people with physically demanding jobs or those who just find stockings genuinely uncomfortable, that two-week stretch can feel longer than it sounds.
VenaSeal often skips the stockings altogether. Post-procedure discomfort is typically lower because there’s no heat involved. That makes recovery feel more straightforward for many patients.
The trade-off? VenaSeal costs more. The adhesive material drives up the price, and that gap is noticeable. It is also not the right fit for every anatomy. Veins that sit very close to the skin surface can react to the glue, causing local irritation. There is also a small but real risk of hypersensitivity or allergic reaction to the adhesive – worth discussing honestly with your doctor before you commit.
Radiofrequency ablation treatment, by contrast, is widely available and generally more affordable. It works well across most vein types and most patients, with decades of practitioner experience behind it.
So Which One Makes Sense?
There’s no clean universal answer, and anyone who gives you one without examining your veins first is moving too fast.
RFA treatment for varicose veins makes sense if you want a well-documented treatment with a long outcome history, lower cost, and broad applicability. The compression stocking requirement is manageable for most people, and the success rate speaks for itself.
VenaSeal makes sense if post-procedure comfort is a real priority for you, if you have a lifestyle or job that makes wearing stockings difficult, or if heat-related risk concerns you. Just go in knowing it costs more and carries a small adhesive sensitivity risk.
Some patients end up with a combination of both, depending on how many veins need treatment and where they sit anatomically. That’s not unusual. It is just a more complex vein presentation requiring a more tailored plan.
The honest starting point is a proper vein assessment. Knowing which veins are affected, how deep they run, and what your medical history looks like shapes the decision more than any general comparison chart can.If you are looking for experienced vein care, the team at Advanced Cardiovascular Center can walk you through both options, assess your specific anatomy, and help you figure out which approach actually fits your situation – not just the general case.